Did you know that an estimated 15 million root canals are performed every year? With so many root canals being performed on an annual basis, you likely know someone who has had one. In some cases, you may have even had one yourself or may be wondering if you need one. As a general rule of thumb, root canals are generally only performed when other restoration methods are not enough to prevent the tooth from falling out or being extracted due to a pulp infection.
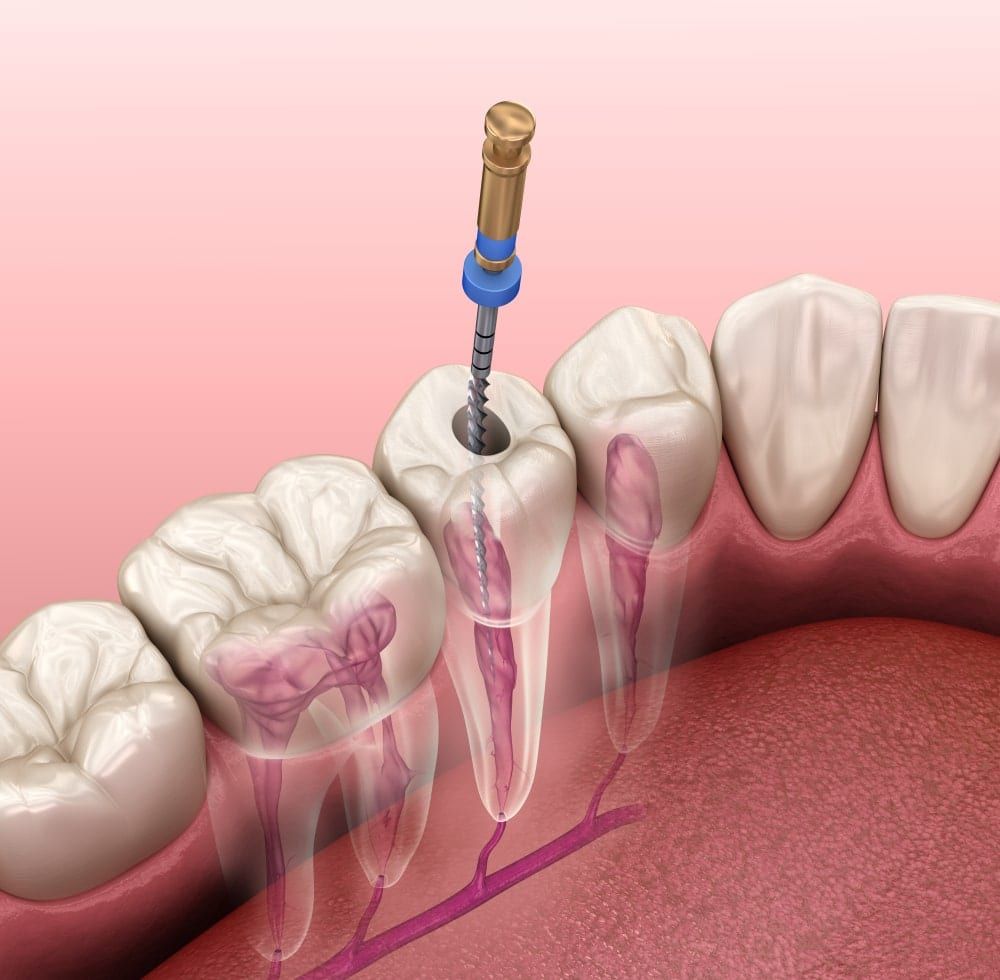
Then dental pulp is the innermost layer of the tooth and is composed of blood vessels and the tooth nerve. Pulpitis, or a pulp infection, can occur whenever bacteria is able to enter the inside of the tooth. One common cause of pulpitis is severe tooth decay that erodes through the enamel and dentin to reach the pulp. However, pulpitis can also occur when the tooth becomes broken or fractured, as well as when faulty or old restorations fail.
In order to prevent the infection from spreading to the surrounding teeth, a root canal is performed to remove the infected tissue, as well as the blood vessels and tooth nerve. The pulp chamber and root canals are then flushed with an antimicrobial solution to reduce the risk of future infection. Once all the infected tissue has been removed and the inside of the tooth has been thoroughly cleaned, the affected tooth will then be restored.
If you have a pulp infection, then you can expect your dentist will recommend having a root canal performed to remove the infection. Here are some possible signs that you may need a root canal:
Toothache
If you start to experience a sudden toothache that continues to get progressively worse, then you may need a root canal. Toothaches associated with pulpitis are described as being a deep, throbbing pain in the tooth that can spread into the jaw. In some cases, this pain is constant, while in other cases, the pain will come and go. It is also common to experience increased pain whenever pressure is applied to the tooth or while chewing. Finally, toothaches associated with pulpitis are also usually accompanied by prolonged tooth sensitivity. Tooth sensitivity is a sharp, deep pain that occurs when the tooth is exposed to hot, cold, or sweet stimuli. With prolonged tooth sensitivity, however, this pain will continue even after the source has been removed from the tooth.
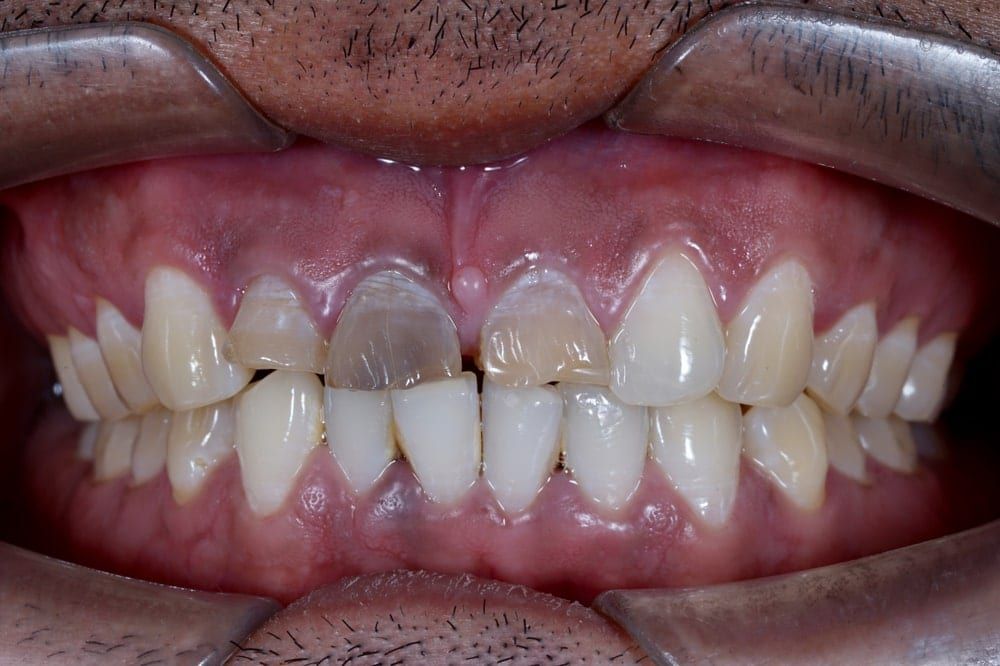
Discoloration
If you have noticed that one of your teeth is suddenly a different color than the rest of your teeth, then you may need a root canal. A single discolored tooth can be a sign of a pulp infection in cases where the tooth appears yellow, gray, light brown, or black. These colors can appear when the pulp infection inside your tooth has started to kill the pulp tissue. The only way to fix this discoloration is to remove the infected and decayed tissue using a root canal.
Gum Issues
If you suddenly notice gum problems around a specific area, then you may need to have a root canal. This is because the same bacteria that cause pulpitis can spread to the gum tissue around the affected tooth. This can cause the gums around the affected tooth to become red, swollen, or tender. In some cases, it can also cause pimples or discharge to form along the gum line. If the infection continues to spread, then gum disease can spread throughout the mouth.
To sum it all up, if you start to experience a sudden toothache, tooth discoloration, or gum issue, then you may need to have a root canal. However, only your dentist can diagnose a pulp infection and the need for a root canal. In some cases, these symptoms could be indicative of another issue. It is also important to note that some pulp infections do not cause symptoms and can only be detected through dental x-rays. Nevertheless, if you are diagnosed with a pulp infection, then you will need a root canal to preserve your tooth.

Dr. Sarmad Channo, a Rochester, MI dentist, received his doctorate degree from New York University Dental School. Since then, he has continued studying to broaden his expertise and has also graduated from Progressive Orthodontic Seminars with the highest of honors. Dr. Channo has also served as an instructor for both the McGann Postgraduate School of Dentistry and Progressive Orthodontic Seminars.

